
Healthcare & Payer
AI for Health Plans and Payer Organizations
Composable, regulated-ready intelligence that turns data chaos into trusted, actionable knowledge — deployed securely, with zero hallucination and full explainability.
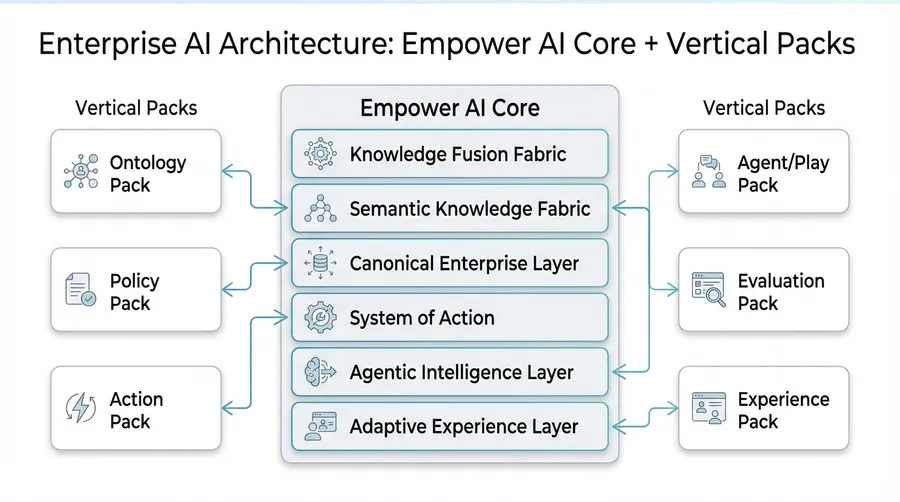
The Empower AI Difference
Empower AI transforms fragmented, legacy-bound organizations into knowledge-driven enterprises. Unlike vendor-tied AI, it is agnostic, composable, and non-hallucinating — built for regulated deployments where trust and traceability are non-negotiable.
Trusted AI with Full Provenance
Every response is grounded in verifiable sources with traceable reasoning. No hallucination. No probabilistic guessing. Audit-ready by default.
Semantic Data Unification
Federates data across health systems, claims platforms, provider networks, and member databases into a unified semantic fusion fabric — without requiring core system replacement.
Explainable Automation
Automates complex workflows (claims adjudication, compliance monitoring, fraud detection) with full transparency into how decisions are made.
Composable Integration
Works alongside existing Salesforce and Microsoft ecosystems, enriching them with factual, domain-grounded intelligence rather than replacing them.
Expected Outcomes
| Metric | Expected Impact |
|---|---|
| Claims Processing Speed | 30-50% faster |
| Manual Compliance Checks | 40% reduction |
| Fraud-Related Losses | 20% reduction |
| Time to ROI | 6 months on initial pilot |
| Member Satisfaction | Improved through faster, more accurate service |
| NCQA Ratings | Improvement through proactive compliance and quality management |
The Challenge for Regional Health Plans
Fragmented Systems
Claims, provider, and member domains live in disconnected systems with inconsistent data models. Cross-domain insights require manual reconciliation.
Poor Data Quality
Unstructured or incomplete datasets limit actionable intelligence. Traditional analytics tools cannot reason over messy healthcare data.
Regulated Environment
HIPAA, CMS, and NCQA requirements constrain technology deployment. Generic AI tools lack the governance infrastructure.
Slow Time-to-Market
New programs, compliance updates, and process changes take months to deploy through traditional channels.
Vendor Dependency
Vendor-provided AI layers lack domain reasoning, healthcare-specific knowledge structures, and deployment flexibility for regulated operations.
Priority Use Cases
Claims & Pre-Authorization Automation
Extract, validate, and auto-adjudicate claims with rule-aware, explainable automation. Impact: 30-50% faster claims processing with reduced error rates.
Compliance Intelligence
Continuous HIPAA and NCQA monitoring with proactive audit readiness. Impact: 40% fewer manual compliance checks.
Member & Provider Assistants
AI-powered copilots for call centers, brokers, and staff that deliver factual, provenance-backed responses to inquiries.
Data Fabric & Cross-System Insights
Unify data across owner health systems and partner networks to generate actionable, cross-domain analytics.
Fraud Detection & Risk Monitoring
Pattern recognition across claims and provider data to identify anomalies and automate investigation. Impact: 20% reduction in fraud-related losses.
IT Modernization Assistant
Assess and document legacy systems for migration planning. Map dependencies, identify risks, and generate migration roadmaps.
Why Not Vendor AI?
Unlike Salesforce Einstein or Microsoft Copilot, Empower AI is not tied to a CRM or productivity suite. It focuses on regulated reasoning, knowledge provenance, and safe automation.
| Dimension | Vendor AI | Empower AI |
|---|---|---|
| Scope | Bounded by vendor platform | Agnostic across all systems |
| Domain Reasoning | Generic | Healthcare-specific ontologies and policies |
| Hallucination Risk | Present | Eliminated through provenance-grounded reasoning |
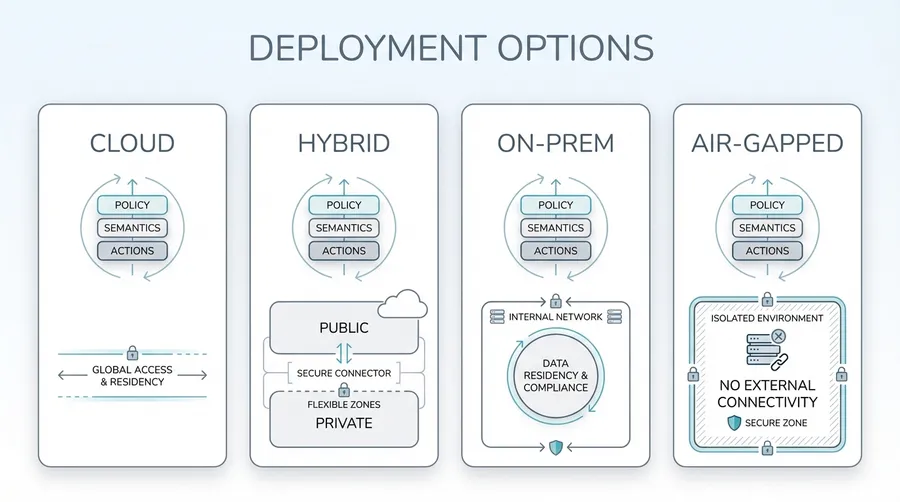
| Deployment | Vendor cloud | Customer's HIPAA-secure environment |
| Explainability | Limited | Full decision traces and audit trails |
| Integration | Within vendor ecosystem | Composable across any system |
Ready to see it in action?
See how Empower AI can transform your health plan operations.